DIAGNOSING AS AND NR-AXSPA
Ankylosing spondylitis (AS) and non-radiographic axial spondyloarthritis (nr-axSpA) can be hard to diagnose. There is no definitive test that results in an AS or nr-axSpA diagnosis. And, because people with AS or nr-axSpA often think their pain is "mechanical"—the kind caused by physical strain to the back—instead of chronic and inflammatory, their symptoms can go undiagnosed for a long time.

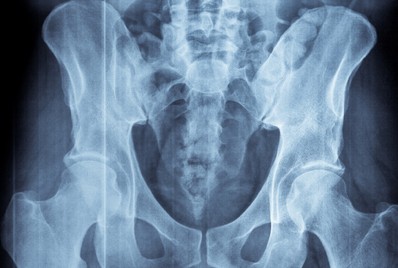

Diagnosing ankylosing spondylitis or non-radiographic axial spondyloarthritis involves:
- Imaging tests, which may include:
- X-rays of your joints and bones
- An MRI, which uses radio waves and a strong magnetic field to provide detailed images of bones and soft tissues
With ankylosing spondylitis, structural damage to the spinal joints is visible on an X-ray (or "radiograph").
With non-radiographic axial spondyloarthritis, there is no clear evidence of inflammation on an X-ray. However, inflammation can sometimes be detected on an MRI.
- A physical examination of your joints and spine to look for signs of ankylosis (fusion) of the spine—also known as “bamboo spine.” Your doctor may:
- Test your range of motion
- Ask you to take a deep breath to check for difficulty expanding your chest
- Individual medical history
- Family history of ankylosing spondylitis and/or non-radiographic axial spondyloarthritis
- Blood work to test for a genetic marker called HLA-B27
While having the HLA-B27 gene doesn’t mean you have AS, it can be an important clue. Many people have the HLA-B27 gene and don’t have AS or nr-axSpA.
Why see a rheumatologist?
Ankylosing spondylitis and non-radiographic spondyloarthritis are conditions with very similar symptoms. Because these diseases are already difficult to diagnose, and are so similar to each other, it's important to see a rheumatologist, the most qualified doctors to diagnose them. Rheumatologists are doctors who are specially trained to diagnose and treat inflammatory diseases like AS and nr-axSpA. Talk to your doctor to find out if you should see a rheumatologist.
Mechanical vs inflammatory back pain
MECHANICAL
Usually caused by physical strain to the back (e.g., a sprain or muscle pull)
Typically recognized by pain that:
- Lasts fewer than 3 months
- Feels better with rest
- Can begin suddenly
INFLAMMATORY
Caused by the immune system attacking healthy tissue, resulting in inflammation in the joints of the spine
Typically recognized by pain that:
- Lasts longer than 3 months
- Feels better with exercise
- Worsens and spreads to other areas of the body over time
Talk to your doctor if you’re experiencing any of the symptoms in the table above. Only your doctor can diagnose the type of back pain you’re suffering from.
FACE THE FACTS
THERE MAY BE OTHER
SIGNS OF AS AND NR-AXSPA
If you have any of the following problems, in addition to back pain and stiffness, they could be helpful for your doctor to know when ruling out or diagnosing AS or nr-axSpA.

Family history of AS or nr-axSpA

History of uveitis or iritis
(inflammation of the eye)

Frequent gastrointestinal issues

Itchy, flaky skin rashes

TAKE THE SYMPTOM QUIZ
Find out if your back or neck pain and stiffness could be ankylosing spondylitis or non-radiographic axial spondyloarthritis and then talk to your doctor about your symptoms.

FIND A RHEUMATOLOGIST
If you have AS or nr-axSpA symptoms, talk to your doctor, who may refer you to a rheumatologist.